What Is Psoriasis?
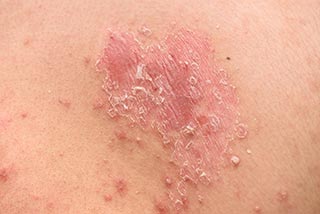
Psoriasis is a skin condition that affects around 2-3% of all people in the UK. It can affect almost any part of the body and is caused by an abundance of skin cells that regenerate the skin too quickly. It can occur on the skin and around joints. Although it isn’t significantly threatening to your health, it can lower your self-confidence or self-esteem and can make you feel unattractive if you have it. It usually affects your arms, feet, and scalp; however, it can also affect the genitals and other body parts.
Psoriasis can cause the skin to become red, flaky and itchy. The key is to find a natural solution as soon as possible and to avoid aggravating the situation further.
What Causes Psoriasis?
Contrary to popular belief, psoriasis is caused not by a skin allergy, but due to an abundance of skin cells that regenerate too quickly. On average your skin should generate new cells every 21-28 days, however when psoriasis strikes, your skin is reproducing cells every few days. This causes cells to build up and leads to plaque on the skin surface, which appears red. It can be very uncomfortable and may also cause you to experience a burning or itching sensation along with scaly skin.
These overacting cells are known as ‘T-Cells’. They basically work as if they were healing a wound (hence their overacting). This skin imperfection is also known as an immune mediation condition or as an autoimmune disease. Although there has been research to identify the cells, it’s still unclear as to why these T-Cells begin working as they do in the first place.
Tips To Help prevent Psoriasis
Limit sun exposure by avoiding sunburn that can lead to new psoriasis infections
Limit the number of baths and the time you spend in the shower. Don't stay in the shower for more than 10 minutes and choose warm water. Use natural products that don't irritate the skin and moisturise after shower.
Take regular physicals, maintain a healthy weight, and control stress levels
Avoid tight clothing, synthetic fabrics as they may irritate the skin. Restrict consumption of tobacco and alcohol too
Impetigo
Impetigo is a scaly skin infection in which one or many blisters filled with pus appear on various parts of the body. The blisters may often be painful with yellowish crusts that start appearing on arms, legs or face and may affect the groin and armpits in a few cases. The infection isn't serious but is highly contagious and hence, requires immediate attention.
What Is Impetigo?
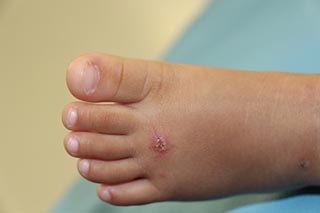
Impetigo is a bacterial skin infection that can affect many adults and the most common cause of this infection is Staphylococcus and Streptococcus bacteria. The infection is highly contagious and spreads through simple physical contact. Sharing personal items like clothes, towels and other such objects can also lead to the spreading of the infection.
Types Of Impetigo
There are mainly 2 types of impetigo – bullous and non-bullous impetigo. In case of bullous impetigo, fluid-filled blisters appear on the arms, legs and trunk. These blisters are usually painless, but are surrounded by red skin that itches extensively. On the other hand, non-bullous impetigo causes sores that burst to leave a yellow-brown crust. The sores also aren't painful in this type as well, but they can be itchy.
Sometimes in rare cases, this bacterial infection can develop into ecthyma, which infects skin deeply. In ecthyma, small pus-filled ulcers are seen with scaly skin. The crust is darker and thicker and there are chances that this type can leave permanent scars. Impetigo generally starts with a single spot that may spread due to scratching and become a rash. Sores of impetigo may sometimes be mistaken for herpes but in such cases, remember impetigo spreads faster and isn’t confined to one area like warts.
How To Manage Impetigo?
The key to impetigo treatment is immediate attention. As soon as you see sores appearing, you must start using an impetigo topical solution. After using a topical solution on daily basis you'll see the sores will begin to fade. The sores of impetigo take time to heal and hence, you must keep using the treatment until they lighten or fade.
In case you're not sure about the infection, make an appointment with a doctor for diagnosis. While you're using a treatment solution, maintaining personal hygiene is indispensable. Take a bath or shower regularly and wash sores with soap and water. It's better to use antibacterial soap to wash the hands and body. As the infection is contagious, it's also advised that if 1 person in a house gets the infection, other family members must start taking precautions.
Seborrhoeic Dermatitis
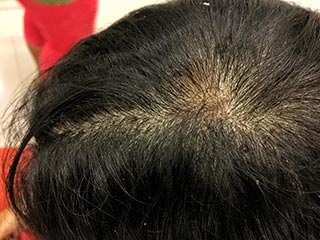
Of all the skin conditions that cause scaly rashes, seborrhoeic dermatitis is a non-contagious condition affecting millions of people a year. Seborrhoeic Dermatitis is a skin condition that affects the scalp and the sebum rich areas of the face and torso. It may appear like bad dandruff and the itching and dryness can lead to scaly skin and rashes. It affects not just adults but babies too wherein the condition is known as cradle cap. Whilst it's common on the scalp, crusty yellow or brown scales can also appear on your face, chest, buttocks, groin, near the navel, below the breasts or in the folds of the skin under your arms and legs.
Causes Of Seborrhoeic Dermatitis
Seborrhoeic dermatitis isn't a result of any allergy. It's easy to mistake it as a diaper rash in babies, or look moist and oily and can cause itching and burning. It can be caused by certain yeast, or medications. Your genes or history of this infection and stress can also contribute to the scaly skin. Cold or dry weather and oily skin can also aggravate the condition. Seborrhoeic dermatitis can additionally flare up in those with a weakened immune system.
How To Manage Seborrhoeic Dermatitis?
Seborrhoeic Dermatitis may become a lifelong condition in many cases. It can heal but then flare up again with just a few triggers. A good skincare routine can help control and prevent scaly skin and using anti-dandruff shampoos is one of the easiest ways to tackle the problem. If the scaly skin patches are too hard or crusty, applying baby oil or another gentle oil can help soften it so that it can peel off during a wash. For Seborrhoeic Dermatitis on other parts of the body, cleaning them regularly with a gentle soap and water has proven to be beneficial. Sunlight can also stop the growth of the yeast hence it's advised to expose the scaly skin to sunlight but only after applying a good sunscreen.
There are a wide range of anti-fungal treatments available to manage Seborrhoeic Dermatitis. To keep scaly skin in control, you'll need to use an anti-dandruff shampoo at least once a week and use good quality moisturisers to help keep the skin hydrated and supple. This will help prevent a reoccurrence of the infection.
Eczema
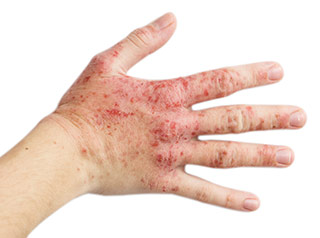
Eczema is marked by itchy, scaly skin that appears red and inflamed. It's commonly known as dermatitis and can lead to cracking, peeling and blistering of the skin. Change of weather, stress, fabrics and even foods can trigger this condition. You can read in detail about Eczema and ways to manage it here.
Tips To Prevent Scaly Skin
Scaly skin isn't just caused by the above mentioned skin infections. It can be a result of a lack of fluids in the body as well as ageing, bathing too frequently or even the environment. You can also experience some discolouration of the skin along with itching, flaking and scaliness. Here’s how you can prevent your scaly skin from turning dry and looking unappealing:
- Don’t bathe too often during the day since it depletes the natural oils from the skin and also avoid using harsh soaps or body washes while bathing. Warm or hot water can also rob the oils from your skin so opt for cool or lukewarm showers.
- If you're tempted to wash the itchy and scaly skin for temporary soothing, avoid it as it can cause further dryness, itching and scaly skin.
- Keep your body and skin hydrated by increasing your intake of fluids in all weathers to prevent scaly skin. Adding omega-3 fatty acid-rich foods can improve the natural oil content of the skin and makes it more supple.
- Identifying the triggers that cause scaly skin and keeping them at bay is also a good way to manage the condition.
The Final Word
Remember scaly skin can happen to nearly anyone. but you can easily deal with it too. Using the right products immediately after being diagnosed with the condition can expedite healing. Maintaining a good skincare routine and using natural products prevents itchy, scaly skin and regular usage will prevent repeat flare-ups.

